
Surgery is the treatment of choice for many skin cancers, including all melanoma, squamous cell carcinomas and some basal cell carcinoma. It is often a simple day procedure done in the clinic.
There are many surgical options depending on the type, size and location of the skin cancer. Local anaesthetics are injected to numb the area prior to any procedures.
YOUR OPTIONS
Curettage & cautery
This procedure involves scooping (curettage) of the skin cancer, using a sharp spoon-shaped instrument. Following this, the base of the skin is burned with low-level heat (cautery) to destroy remaining cancer cells and stop the bleeding. The wound is then covered by a dressing and heals on its own within a few weeks. A small, round, flat and white scar remains.
Curettage & cautery are often used to treat superficial basal cell carcinomas (BCC) and intraepithelial carcinoma (IEC) with high success rates.
Excision and skin flap
For skin cancers where bigger skin areas need to be removed, the large resulting defect will need to be covered with a skin flap or graft.
A local skin flap is healthy skin tissue that is lifted from a nearby area and moved to cover the skin defect after excision. It is still attached to its original site at one end. There are different types of local skin flaps depending on the location and size of the defect.

Transposition Flap from Clinical Gate

Rotation Flap from Science Direct

V-Y Advancement flap from Entokey
Excision and primary closure
After numbing the skin with local anaesthetics injection, the skin lesion is excised (cut out) with appropriate margins of healthy surrounding skin.
The remaining defect in the skin is then closed with stitches. The sutures on the skin surface are to be removed within 1-2 weeks.
Primary closure is straightforward and often used when the defect is small or when the surrounding skin is loose enough to bring together directly.
Excision and skin graft
A skin graft is healthy skin that is removed from one area of the body to cover the skin defect after excision. It is completed detached from its donor site (area where skin is taken from).
There are two types of skin grafts:
- Full thickness graft: thicker skin graft where the donor site will need to be closed with sutures.
- Split thickness graft: thin skin graft where the donor site will heal ones its own
Advantages of split thickness graft are it covers are large area. Disadvantages are the donor site will leave more obvious scars.
Advantages of full thickness graft are it better represents skin, so are often used for skin defects on the face. Disadvantages are they are limited in their size.
Complications of skin surgery
- Bleeding: A small amount of bleeding is expected. Usually this is absorbed by the dressing. Dressing changes may be needed. External pressure for 20 minutes will stop the majority of minor bleeds. Rarely, bleeding is more profuse, and may require reopening the wound, and identifying bleeding blood vessels.
- Infection: There is a small risk of infection following any surgical procedure, usually localized. Antibiotics may be required.
- Distortion of anatomy: Sometimes pulling of the skin close to a wound can cause distortion of nearby structures. This is most problematic on the face, especially around the nose, eyes, and mouth. Your doctor will usually anticipate possible distortion, and design the surgery to minimize this chance.
- Pain: There will be some pain after the local anaesthetic wears off. Usually simple over-the-counter analgesics will suffice. Sometimes stronger pain-killers are needed, especially for large procedures on the head and neck. Pain usually settles within a few days. Very rarely, atypical pain syndromes, which are unpredictable, can occur following any surgical procedure.
- Numbness: There will be some numbness beyond the surgical excision. This usually improves over months. Sometimes it never fully recovers.
- Incomplete excision: Skin cancers extend a distance beyond the visible lesion. A margin of clinically normal skin is also excised, to account for this. Uncommonly (<5%) the subsequent histology (microscopic analysis), shows skin cancer extending to, or close to, the edge of this margin, suggesting there is residual skin cancer. Further treatment may then be required.
- Dehiscence: Sutures are used to hold the wound together. Occasionally these can break, and the wound can “pop-open”, and may need to be re-stitched. This is more problematic for wounds on the lower limbs and back. Remember, sutures are not as strong as you are, and a period of reduction in activity is usually recommended.
- Suture spitting: Buried sutures are usually used. These dissolve on their own. Sometimes before they dissolve, the body pushes them to the surface, and this may be uncomfortable. Whilst it will resolve on its own with time, this can easily be trimmed by your doctor if it occurs, and it is annoying to you.
- No residual skin cancer seen: Sometimes previously biopsied (proven) skin cancer is subsequently excised, and histology does not show residual skin cancer. This is actually good news. The preceding biopsy is not curative, and there is almost always tiny foci of disease, but due to technical reasons, the processing of the specimen may mean that the residual skin cancer is not seen. The margin of normal skin is needed for a high chance of cure.
- Unexpected histology results: Rarely, what clinically looks like a skin cancer, and is excised, turns out to be benign (harmless).
- Scars: There will be a scar. Sometimes scarring is atypical, and abnormal scarring can occur (hypertrophic scarring and keloid scarring). Whilst sometimes abnormal scarring can be anticipated (certain sites, people with a history of poor scarring), unfortunately it may be unpredictable. Further treatment may help abnormal scars, and this may involve additional costs of treatment. A “spread scar” (stretch scar) is expected at certain sites, especially the back and thighs. Certain techniques, and prolonged taping support can reduce this, but at certain sites it will occur to some degree.

- Hypertrophic scars: raised scars that do not spill over the wound edges. Usually improves over time but some treatments can help such as silicone sheets, pressure dressings, injection of corticosteroids, laser and surgery.
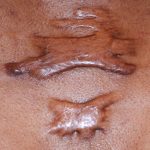
- Keloid scars: large scars that grow over the wound edges. More common in African or Asian descent. These may be reduced by injection of corticosteroids, applying silicone sheets, freezing, laser or surgical removal.

